The Latest in Diverticulitis Management Strategies
Navigating Diverticulitis: Insights from Expert Perspectives
Introduction
As an acute care surgeon, the management of diverticulitis is a common aspect of my practice. The following insights from an expert panel at the 2023 Clinical Congress of the American College of Surgeons shed light on evolving strategies in the field.
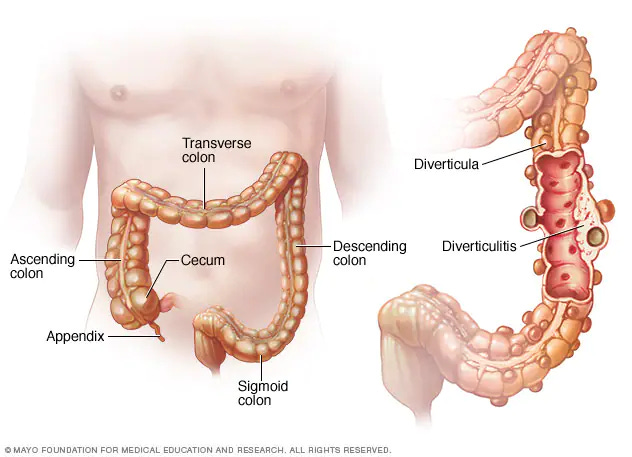
Antibiotics Still Overused in Diverticulitis
Dr. Marylise Boutros emphasized the need to reconsider the routine use of antibiotics for uncomplicated diverticulitis. Despite evidence suggesting limited benefits, the practice persists due to various concerns and traditions within the medical community.
Leading Change
Surgeons are urged to spearhead initiatives aimed at educating both colleagues and patients about the appropriateness of antibiotic therapy. Institutions and professional societies are also called upon to support efforts in curbing antibiotic overuse through advocacy and educational campaigns.
PAPD Slowly Gaining Steam For Diverticulitis
Dr. Robert N. Goldstone discussed the gradual shift towards primary anastomosis with or without proximal diversion (PAPD) as an acceptable alternative to Hartmann’s procedure. This transition is driven by accumulating evidence and increasing surgeon comfort with the procedure.
The decision to perform PAPD versus Hartmann’s should be tailored to each patient's clinical status and the surgeon's expertise. Factors such as perioperative risk and intraoperative considerations play a crucial role in selecting the most appropriate surgical approach.
The Challenge of Immunocompromised Patients
Dr. Dana M. Hayden highlighted the complexities of managing diverticulitis in immunocompromised patients, emphasizing the need for individualized approaches. Factors such as disease severity and patient comorbidities significantly influence treatment decisions.
Addressing Risk Factors
Various patient factors, including the use of steroids and chemotherapy, impact outcomes in immunocompromised individuals. Surgeons must carefully weigh the risks and benefits of different treatment strategies to optimize patient care.
Racial Disparities in Diverticulitis
Dr. Hanjoo Lee addressed the alarming racial disparities observed in diverticulitis outcomes, underscoring the need for concerted efforts to bridge the gap. Disparities in access to care, treatment modalities, and surgical interventions contribute to disproportionate outcomes among minority populations.
Collaborative Solutions
Closing the racial disparity gap requires multifaceted interventions involving governmental and private sector collaboration. Efforts aimed at improving access to healthcare, enhancing provider diversity, and fostering inclusive care environments are essential in addressing systemic inequities.
Conclusion
In summary, the management of diverticulitis continues to evolve, driven by advances in evidence-based practice and a growing recognition of disparities in care. Surgeons play a pivotal role in advocating for patient-centered approaches, fostering interdisciplinary collaboration, and advocating for equitable healthcare delivery.
Hot Take Summary:
The management of diverticulitis is undergoing a paradigm shift, with a greater emphasis on evidence-based practice, individualized patient care, and addressing systemic inequities. Surgeons must lead efforts to optimize treatment strategies, promote antibiotic stewardship, and advocate for equitable access to care to ensure optimal outcomes for all patients.